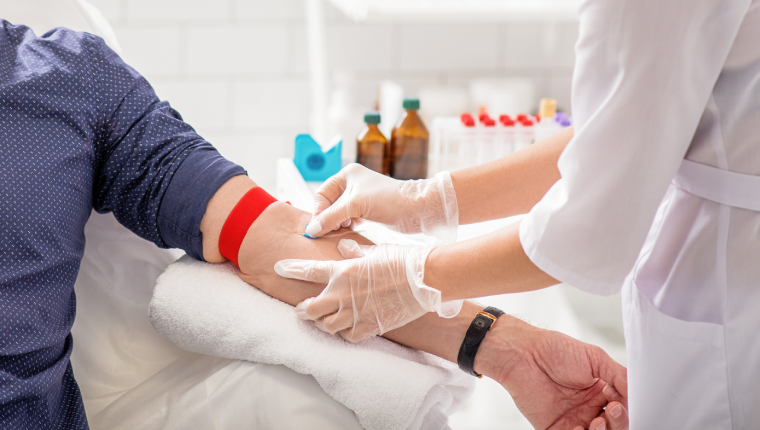
Insulin resistance often develops quietly, sometimes years before blood sugar levels rise or a person is diagnosed with prediabetes or type 2 diabetes. Because it can be difficult to recognize early on, many people don’t realize they may be at risk until more noticeable symptoms appear.
To help you understand how insulin resistance affects the body, what causes it, and how it can be identified early, we spoke with Dr. Margery Connelly, PhD, MBA, FAHA, strategic director of diagnostics research and development at Labcorp. Below, Dr. Connelly explains the science behind insulin resistance, common misconceptions, and how an advanced insulin resistance test can empower you to take action sooner.
How does insulin resistance affect the way the body uses and regulates blood sugar?
Normally, insulin binds to receptors on cells in muscle, fat, and the liver, signaling those cells to use glucose from the blood for energy.
“When these tissues become insulin-resistant, the insulin signal is blocked,” explains Dr. Connelly. “As a result, glucose stays in the bloodstream instead of being used by the cells, which can lead to higher circulating blood sugar levels over time.”
In the early stages, the body often compensates by producing more insulin. Over time, however, this compensation may no longer be enough—setting the stage for prediabetes or type 2 diabetes.
How early can insulin resistance develop before changes in glucose or A1c are detectable?
Insulin resistance is not something that appears overnight. It’s a gradual and progressive process.
“Insulin resistance is continuous, meaning it can increase over time,” says Dr. Connelly. As it gets worse, glucose may rise gradually. However, in some people, it can lead to a sharp increase in glucose.
“Because of this variability, it can be hard to predict exactly when blood sugar or A1c levels will begin to change,” explains Dr. Connelly.
This is one reason insulin resistance can go unnoticed for years and why early assessment may be helpful for long-term health planning.
Why might someone have normal glucose levels but still have high insulin resistance?
Normal glucose levels don’t necessarily mean your body has a healthy insulin response, says Dr. Connelly.
“Insulin resistance comes before blood glucose rises,” she explains. “Some people may have increased insulin resistance before they see an increase in their blood sugar levels.”
During this phase, the body is working harder to keep blood sugar stable by producing more insulin, masking underlying metabolic stress.
What are the limitations of relying on fasting insulin alone to understand insulin resistance?
Fasting insulin levels can provide some information, but they don’t tell the full story.
“Fasting insulin changes throughout the day, as well as during and after meals,” says Dr. Connelly. On its own, it doesn’t necessarily tell you whether insulin levels are unusually high for your body.
“Fasting insulin and glucose alone are not always good indicators of insulin resistance, especially in individual patients, because they can vary a lot between people as well as within each person.”
What does the LP IR Index measure, and why is it clinically meaningful?
The Lipoprotein Insulin Resistance Index (LP IR) looks beyond glucose and insulin levels.
“The LP IR measures changes in six lipoprotein markers that indicate when a person has insulin resistance,” explains Dr. Connelly.
Because insulin resistance affects how the body processes fats (i.e., lipoproteins), these lipoprotein patterns can reveal metabolic changes that happen well before blood sugar levels rise—making LP IR a valuable early indicator of risk.
How does the LP IR score (0–100) relate to the risk of type 2 diabetes?
LP IR scores range from 0 to 100, with higher scores suggesting greater insulin resistance. “Scores of 68 or above indicate a higher risk of progressing to type 2 diabetes,” explains Dr. Connelly.
A lower score suggests better insulin response, meaning your body is more sensitive to insulin and only needs a small amount to manage blood sugar—generally a good sign of metabolic health.
This score can help identify risk earlier, before traditional markers like glucose or A1c become abnormal.
Who should consider getting an insulin resistance test?
According to Dr. Connelly, insulin resistance testing can be valuable for a wide range of people.
“Anyone who wants to learn more about progressing to type 2 diabetes or their risk of heart disease should consider an insulin resistance test,” she says.
This can be especially helpful for those focused on weight management or fitness changes, people interested in understanding cardiometabolic risk beyond standard glucose testing, or individuals with risk factors for insulin resistance, such as:
- Family history of diabetes
- High blood sugar levels
- High triglycerides (a type of fat in the blood)
- High LDL (“bad”) cholesterol
- Low HDL (“good”) cholesterol
- Physical inactivity
If you have a higher LP IR score, what steps can you take to support better metabolic health?
Insulin resistance can often be improved, especially when identified early.
“Low calorie diets, vegetarian diets, and eating patterns such as the Mediterranean diet, along with increased physical activity, can lead to weight loss, improved metabolic health, and reduced insulin resistance,” says Dr. Connelly.
If lifestyle changes don’t lead to improvement, she recommends consulting a healthcare provider for guidance tailored to individual needs and health goals.
When is repeat testing appropriate? How often should you consider rechecking your insulin resistance score if it is elevated?
Tracking progress over time can be an important part of prevention.
“Insulin resistance scores should be rechecked at least 12 weeks after starting a lifestyle change,” suggests Dr. Connelly. Repeat testing can help assess whether changes in diet, exercise, or other habits are improving insulin sensitivity and overall metabolic health.
Insulin resistance and the importance of early insights
Because insulin resistance often develops silently, having access to advanced testing can make a meaningful difference.
Labcorp OnDemand’s Insulin Resistance Test gives you an advanced look at your metabolic health by estimating your body’s response to insulin. With this information, you and your healthcare provider can take proactive steps toward preventing type 2 diabetes and supporting long-term cardiometabolic health.